 National Heart, Lung and Blood Institute. Process design for optimized respiration identification based on heart Rate variability for efficient respiratory sinus arrhythmia biofeedback. Factors affecting the ST-T and U wave configuration include: Intrinsic myocardial disease (e.g. 2015 ACC/AHA/HRS guideline for the management of adult patients with supraventricular tachycardia. This does not mean that the ECG changes are unimportant It is the responsibility of the clinician providing care for the patient to ascertain the importance of the ECG findings. Diagnosis and management of supraventricular tachycardias. Code R00. Report R00.1 (Bradycardia, unspecified) for sinus bradycardia. This condition is most common in patients who exercise regularly or are over age 65. doi:10.15420/aer.2015.4.1.28īibas L, Levi M, Essebag V. Sinus bradycardia is a type of bradycardia that originates from the sinus node of the heart. Biology of the sinus node and its disease. Bradycardia: slow heart rate.Ĭhoudhury M, Boyett MR, Morris GM. Heart rate greater than 80 as mortality predictor in acute myocardial infarction. Respiratory sinus arrhythmia in the immediate post-exercise period: correlation with breathing-specific heart rate. Mortola JP, Marghescu D, Siegrist-Johnstone R. Canadian Journal of Cardiology, 30(6), 606–611. Predictors of advanced His‐Purkinje conduction disturbances in patients with unexplained syncope and bundle branch block. Journal of the American College of Cardiology, 46(5), 858–863. Prognostic significance of left anterior hemiblock in patients with suspected coronary artery disease. In a study of 6014 healthy men in the U.S. Tracing 1 in Figure 1 is an example of normal ST-segment elevation. Annals of Noninvasive Electrocardiology, 20(1), 7–17.īiagini, E. the T wave during sinus tachycardia or if the PR segment is depressed or there is a prominent atrial repolarization (Ta) wave. Comprehensive review and proposed algorithm. 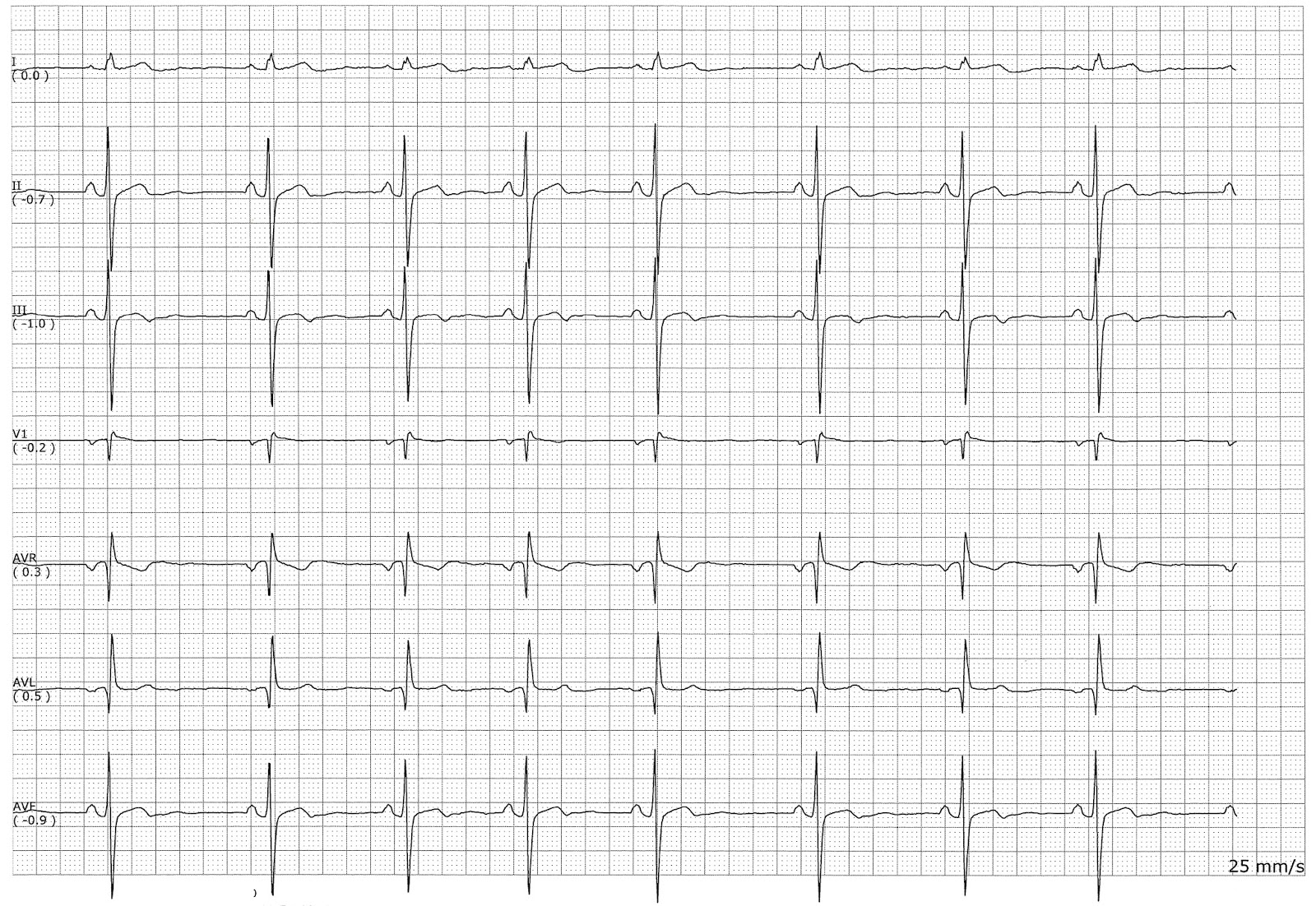
Differential diagnosis of rSr’ pattern in leads V1–V2. Circulation: Arrhythmia and Electrophysiology, 4(5), 704–710. Intraventricular conduction delay in a standard 12‐lead electrocardiogram as a predictor of mortality in the general population. 
Prevalence of manual Strauss LBBB criteria in patients diagnosed with the automated Glasgow LBBB criteria. Annals of Noninvasive Electrocardiology published by Wiley Periodicals LLC.Īlmer, J. The prognostic impact of LBBB and NSIVCD was affected by the definition of the conduction disorder.īundle branch block electrocardiography intraventricular conduction delay population study prognosis. Other IVCDs had no significant impact on prognosis. In a population study with long-term follow-up, NSIVCD and Minnesota definition of LBBB were independently associated with CV mortality. Urgent guidance for navigating and circumventing the QTc-prolonging and torsadogenic potential of possible pharmacotherapies for coronavirus disease 19 (COVID-19). The presence of R-R' pattern was not associated with any adverse outcome. This calculator calculates the heart rate-corrected QT interval and guides prescription decisions to prevent drug-induced QT interval prolongation. While right bundle branch block, left anterior fascicular block and incomplete bundle branch blocks were associated with seemingly higher mortality, this was no longer the case after adjustment for age and sex. Subjects with NSIVCD were associated with twofold to threefold increase in CV mortality depending on the definition. 308) for the Strauss' definition of LBBB. After controlling for known clinical risk factors, the hazard ratio for CV death, compared with individuals without IVCD, was 1.55 for the Minnesota definition of LBBB (95% confidence interval 1.04-2.31, p =. 
For left bundle branch block (LBBB) and non-specific IVCD (NSIVCD), two different definitions were used.ĭuring 16.5 years' follow-up, 1,309 of the 6,299 subjects (20.8%) died and of these 655 (10.4%) were cardiovascular (CV) deaths. We studied long-term prognostic impact and the association with comorbidities of eight IVCDs in a random sample of 6,299 Finnish subjects (2,857 men and 3,442 women, mean age 52.8, SD 14.9 years) aged 30 or over who participated in the health examination including 12-lead ECG. Previous population studies have presented conflicting results regarding the prognostic impact of intraventricular conduction delays (IVCD). 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
